Children are not the face of covid-19 but will certainly not be spared

© MSF, 2020
Children have been more severely affected by the indirect impact of the pandemic than by the virus infection itself. The COVID-19 pandemic has impacted child health through increases in poverty, loss of education, food insecurity, violence as well as increased strain on health systems and reduction in access to health services. These collateral effects of the pandemic have stricken most in resources limited settings where increase in child mortality is a major concern. There is a risk that these collateral effects will be further exacerbated when hundreds of millions of COVID-19 vaccine doses will be rolled out in the latter part of this year in low-income countries. The amount of healthcare workers needed to deliver those vaccines may push away services that we already see are damaged and children will be paying the price for this.
Liliana Palacios, who answers our questions, is a nurse with a master's in Public Health and Structures Management. She currently works as a Health Advisor for MSF Spain, giving support to projects in RDC, RCA and Cameroon. She is also part of the team that developed the “Collateral damage of COVID-19 on child health" session for the MSF Paediatric Days 2021. Liliana reflects on the outcomes of the session and considers the Paediatric Days conference an open space to share and learn.
Can you explain what the objective of the “Collateral damage of COVID-19 on child health" session was?
The session focused on highlighting the impact of the collateral effects of the pandemic on child health and mortality in MSF settings. We wanted to share experiences on how the teams providing paediatric services faced the situation and overcame (or not) the challenges. For that, we carried out a survey among MSF field staff and recorded video testimonies. We were also interested in hearing experiences and stories on this matter, so we invited experts from other organizations and from MSF to participate in the session.
Which child services and programs have been more severely affected by the COVID-19 pandemic?
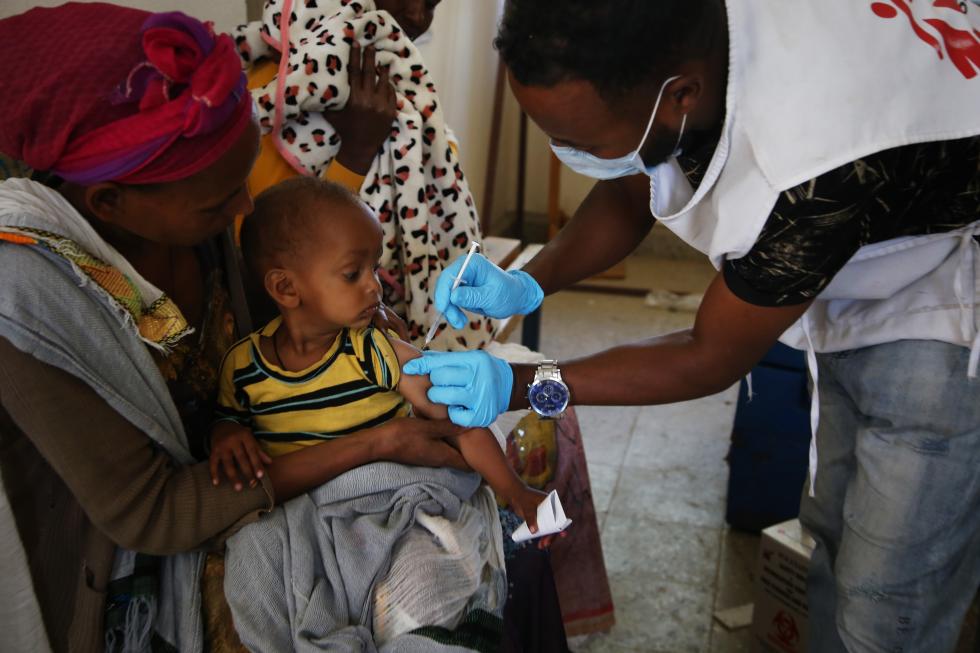
From the beginning of the pandemic, we clearly saw that vaccination and nutrition programs were heavily impacted. At the same time, other basic non-medical services for children have also been affected: access to education, protection against domestic violence, etc.
The health staff also had to be relocated to meet the needs arising from the pandemic. In this type of humanitarian context there is already a limited medical staff, hence by diverting part of the human resources to cover the response to COVID-19, the risk of not meeting basic needs in paediatric programs increased.
The pandemic also impacted the “physical spaces” of other areas such as paediatrics as the increase in demand for beds and isolation units to treat COVID-19 have been prioritized.
© Igor Barbero/MSF, 2021
What are the main recommendations outlined during this session to prevent child morbidity and mortality growth?
The first recommendation is simple, we must maintain the preventive and curative paediatric regular services. Part of the human, material and strategic resources that usually exist for these preventive programs have been reduced and we will see the consequences in the near future. For example, we might see some epidemic outbreaks soon because of the children who have not been vaccinated against rubella or measles. By reducing or closing outpatient clinics, the number of diagnoses (for example the diagnosis of severe malaria) may increase in the future.
Secondly, we should develop new approaches and implement practical tools needed in the field (for example: “Family MUAC” (Mid-Upper-Arm Circumference) nutrition programmes, digital learning opportunities, increased community engagement, etc.)
Lastly, we need to further advocate for children's rights in this pandemic. They are not the ones dying of COVID-19 but will certainly be the ones that are most impacted.
Regardless of the negative impact the COVID-19 pandemic has and will have on children, have there actually been any positive externalities in paediatric projects on the field?
Community health care activities, which have become a key part in addressing COVID-19, have reminded us of the efficiency of this system and should continue to be highly implemented and integrated in MSF operational strategies.
This situation reminded us that we need to be flexible and innovative to provide proper technical support to the field.

© MSF
Can you give a concrete example of good field practice or a successful intervention strategy that was presented during the MSF Paediatric Days? What could we learn from it and could it be implemented in other MSF projects?
The “Family MUAC” project in White Nile (Soudan) has shown good results in other field projects and is a way of ensuring community participation in a more active way. MUAC trains mothers and other caregivers to identify early signs of malnutrition in their children using colour-coded paper bracelets to measure the mid-upper-arm circumference.
To implement this model in Sudan, we used MSF’s previous experience in Congo in 2019. We started executing it in Congo due to the difficulties the population faces to access local health services (because of long geographical distances and violent conflicts). The goal was to enable early detection of malnutrition and reduce admissions of severe malnutrition. It should be noted that the “Family MUAC strategy” is not an invention of MSF: other humanitarian organizations such as ALIMA, UNICEF or Action Against Hunger also have similar programs.
With the COVID-19 current situation, this kind of project works very well. It helps reducing the contact between the health staff with the patients. By moving this task to mothers (or other family members), the cases are detected earlier, leading to less hospitalizations; and families are empowered to manage their children's health. I do think it shows very well how our field programs can be adjusted to keep assuring the main outputs in those places where services for children are very relevant.

© MSF
As a medical professional, why do you feel it is important to participate in conferences such as the MSF Paediatric Days?
Because it is an opportunity to share experiences, learn and debate with other people, which in turn will helps us improve our activities. Listening to other colleagues inspires me and helps me improve my work. The online format has broken down many barriers and connectivity has made it possible to have a wider audience.
The Paediatric Days team thanks Liliana Palacios for her contribution to this article.
