Prevention is better than cure
Malaria is one of the leading cause of child mortality in sub-Saharan Africa with mortality numbers increasing in the past few years. Seasonal or year-round, MSF is fighting the disease with a focus on enhancing prevention methods.

© MSF/Cynthia D'Cruz, Tanzania
Malaria, a disease spread by plasmodium parasite carrying mosquitoes, causes an often-severe infection to the body. The symptoms caused by malaria, include fever, inflammation, and breathing difficulties. It can affect any part of the body, from the brain to the liver or lead to coma or death if left untreated.
“We can see malaria across all ages in most populations where MSF works. The people who are most at risk for having malaria, especially severe cases of malaria, are children” says Kemi Ogundipe, MSF Paediatric Advisor and member of MSF's international Paediatric Working Group.
Kemi Ogundipe has worked in MSF projects all over the world and has seen firsthand the effect malaria has, especially on children.
The severity of malaria rises the younger the patient is, studies show that 77% (2021) of all malaria mortalities were children under five. The symptoms are usually more pronounced in children under five and more severe, often fatal, in children under two. Malaria often causes side effects, some that outlast the infection.
“Typically, there are other things that come along. For younger children, malaria can cause anemia and they will need blood transfusions. When malaria is not fatal, patients can have a hard time recovering fully and may experience some lingering problems, such as seizures, learning difficulties and delays in overall development”.
Every year malaria is the number one cause of fatalities in children under five years old in sub-Saharan Africa. There are effective medications, but the patients and their families might not always have access to them or do not seek treatment until it is too late.
Liliana Palacios, nurse and health advisor in MSF operations department continues:
“One of the challenges to assure early detection and opportune treatment is the access to services, as most of the time they are centralised and families might have difficulties accessing them, because of economic reasons or because the treatment is simply too far to reach”.
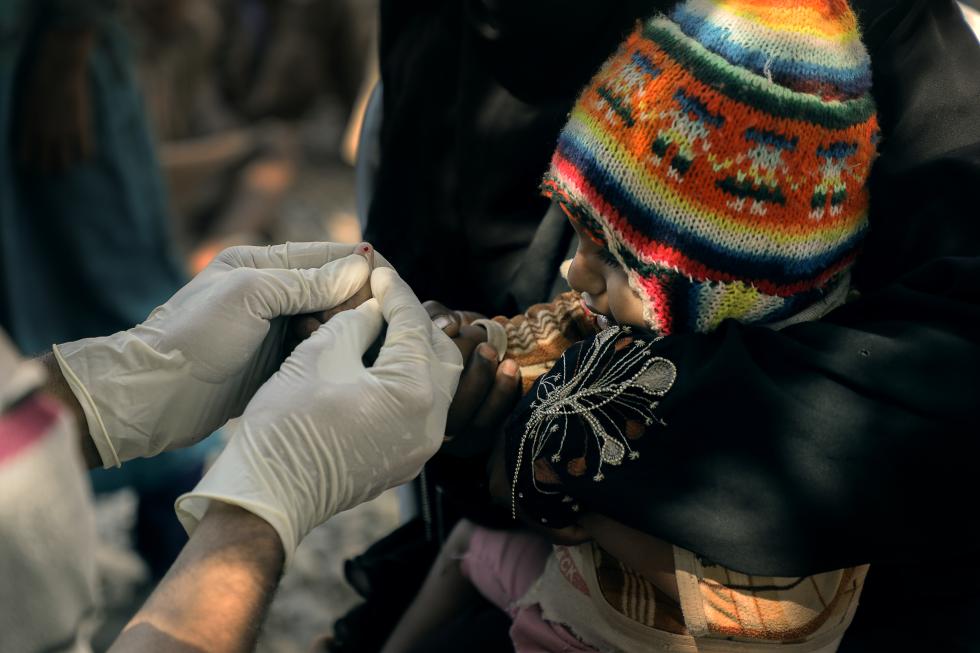
Ehab Zawati/MSF, Yemen
This is one of the key reasons why both Kemi Ogundipe and Liliana Palacios feel strongly about developing effective and widespread malaria prevention tactics and medications.
“We have made some amazing strides in what we can do to treat the patients who have been infected by malaria. The medication is effective, and we are now able to support the patients better when they are sick. But if we were able to prevent malaria from even occurring, we would take a huge burden off the patient and off the community at large”, says Kemi Ogundipe.
Kemi Ogundipe highlights that there are already some prevention mechanisms that have been proven to work extremely well. For example, in the last 20 years, Sri Lanka has been able to eradicate malaria completely. “We have chemoprophylaxis for areas where malaria only occurs for a few months of the year. It prevents children being infected during the risk period with up to 74% efficiency. We also have bed nets, water treatments and sprays... Imagine if you combined all these things, you would avoid malaria occurring in a lot of populations”.
The science on effective malaria prevention tools is continuously developing, still much more conversation, innovation and investment are needed.
“For example, we can see that there is real lack of more effective preventive measures in place – possession and correct use of mosquito nets, for instance, is not always present or promoted efficiently,” says Liliana Palacios. “If we could work in anticipating, facilitating or promoting the early consultation and the application of complementary measures of vector control we could contribute to reduce the number of patients or deaths related to the disease.”

© MSF/Cynthia D'Cruz, Tanzania
Kemi Ogundipe adds: “There is still a lot unknown in terms of prevention and we are limiting our impact, if we only focus on receiving and treating a child or an adult that is sick from malaria. The investment and the conversation should be on prevention if the goal is to avoid children dying of malaria”.
Today we can see that malaria infection numbers are increasing globally partly due to climate change. The disease is now appearing in areas where it has not been met before, as the changing climate is offering more hospitable places for the malaria parasite to live.
Added risks appear also in combination with other diseases as malaria tends to be more fatal when combined with other illnesses. Kemi Ogundipe says that humanitarian medical community was anticipating COVID-19 pandemic to make malaria even more serious of a problem. Luckily, that did not happen in many of the countries where malaria prevention program had been completed.
Kemi Ogundipe: “This shows that if we could avoid malaria completely and put more focus on prevention, we would be more prepared and capable fighting diseases like COVID-19”.
Malaria: Prevention is better than cure will be one of the main sessions during the MSF Paediatric Days 2022.
The MSF Paediatric Days team thanks Kemi Ogundipe and Liliana Palacios for their contribution to this article.
