Fatal first days
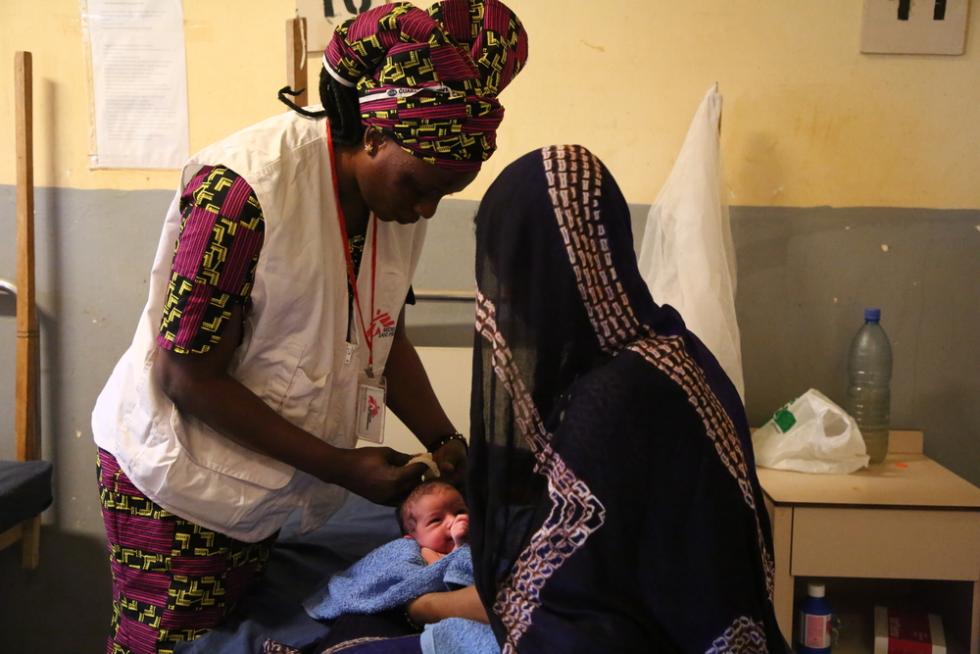
Which are the riskiest days in life? Half of the deaths among children under the age of five occur in the first 28 days after birth. In many places where MSF works, high-tech solutions for the care of newborns are lacking, but a lot can be achieved with relatively simple efforts.
"Nasreen sits on the edge of the bed and holds the small chin and the mask with one hand, the manual resuscitator with the other and stares at the chest. It is day three of the boy's life, and he has fought like a lion to survive, having been born 8-10 weeks early, weighing only 1.6Kgs. Nasreen has been helping him breathe for more than six hours. The hope that the boy will be able to continue breathing on his own is small, but alive. She continues a little, a little while longer.”
This is an excerpt of paediatrician Sanna Sjöberg’s blog post on MSF's website. She and her colleague Nasreen know all too well the challenges that the little boy and other children born prematurely face in Afghanistan, where neonatal mortality is one of the highest in the world.
Half of the patients
In the small town of Khost, located in the eastern part of the country right on the border with Pakistan, MSF runs a large maternal and newborn health hospital.
“When women do not have the opportunity to seek medical care during pregnancy or childbirth, they are at risk of serious conditions with no possibility for diagnosis or treatment. This in turn increases the risk of the babies of these women being born prematurely or with complications,” says Paediatric Advisor Kemi Ogundipe.
She is part of the MSF International Paediatric Working Group, which was created in 2008.
“In most countries where we work, children make up more than half of the patients we see and we have realized that we need to take a focused approach to the paediatric healthcare we provide,” says Kemi Ogundipe.
Midwives are important
Over the past 50 years, the under-five mortality rate has fallen significantly on a global scale. This development can be explained mainly by the improved availability of vaccinations against diseases such as diphtheria, tetanus, whooping cough, measles, rubella, and mumps.
It is also because the methods for preventing and treating malaria have improved, access to clean water has increased and more children receive treatment against dehydration and malnutrition.
“Unfortunately, the death toll among the very smallest has not decreased to the same extent. Newborns account for almost half of all deaths among children under the age of five,” says Kemi Ogundipe.
The main reasons why babies fall sick, or die, are complications resulting from premature births or asphyxia, which means that the baby suffers from a lack of oxygen and insufficient blood circulation. In case of asphyxia, the delivery must be quick and is often managed with forceps, vacuum-assisted delivery or caesarean section.
Kemi Ogundipe emphasises the importance of women receiving regular health checks during pregnancy so that risk factors can be detected early, and problems prevented, something that does not always happen in humanitarian or low resource settings. Well-trained health workers are crucial in the management of premature births and asphyxia. A large part of what the Paediatric working group does is therefore about education.
Premature or sick babies often need help breathing, getting nutrients, and staying warm. In many of the places where MSF works, access to high-tech medical care as in high income countries is not available.
But even if technology is important, much can be done with basic techniques. This is underlined by Mats Blennow, chief physician specialised in neonatology, who has worked for MSF in Jordan and Nigeria.
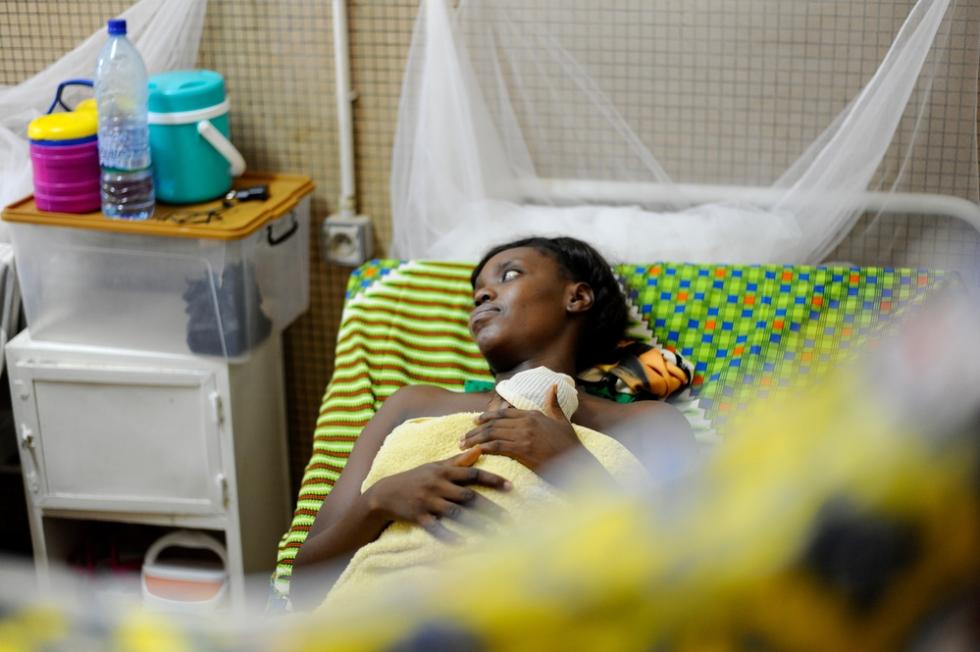
© MSF/ Marco Scardovi, 2020
Healthy skin contact
“Skin-to-skin contact with the mother is crucial for the health of the newborn, as it helps regulate the baby’s temperature and heart rate, helps promote breastfeeding and milk production and helps the baby to stay calm and decrease stress. In Sweden, over the past 30 years we have increasingly invested in family-centred care, assuring that mothers, fathers, caretakers and babies can be together, in the same room, 24/7. In the past, mother and baby were separated and there could be six to seven babies in the same room.
Similarly, it is possible to implement simple strategies in the places where MSF works, where skin to skin has become an important part of care for newborns through kangaroo mother care (KMC). KMC uses locally acquired materials to create a wrap that can safely and securely allow babies to have continuous skin-to-skin contact with their mother, father, or another primary caregiver for over 20 hours every day. This stabilises the baby's breathing and heart rhythm and makes them less susceptible to infection. The method is specifically indicated for low birthweight babies, the World Health Organization (WHO) recommends this for all children below 2 kilograms.
“A large research study was recently released in which KMC was used with premature babies in Ghana, India, Malawi, Nigeria, and Tanzania. The study showed that the newborns had a higher rate of survival,” says Mats Blennow.
Particularly susceptible to infection
The design of the wards for newborns is also important to reduce the risk of transmission of infections, Kemi Ogundipe points out.
“Newborns are extra vulnerable to bacterial infections in the blood, brain, and skin due to their immature immune system. Premature babies are also particularly sensitive to infections in the gut. Babies need to be kept in a closed environment where they are in contact with as few people as possible.
“It is also important to make sure that the wards are cleaned properly, that the staff maintains good hygiene and that there is proper access to clean water.” The importance of these efforts became particularly clear to MSF five years ago when a neonatal unit in Bangui, the capital of Central African Republic, suffered a severe outbreak of sepsis and antibiotic resistant Klebsiella pneumoniae was identified.
“After the outbreak, we introduced warning systems where babies with fever are closely monitored to detect cases of resistant bacteria. We have also ensured that there is more space to isolate patients, that the beds are not put too close together to avoid the spread of infections. All mothers are also given continuous access to clean water to wash their hands and given clean gowns to place over their clothes,” says Kemi Ogundipe.
In recent years, some more advanced care solutions for newborns have become available in low resource settings. One example is Continuous Positive Airway Pressure (CPAP), a non-invasive treatment that uses air pressure to maintain an open airway, decreasing the risk of apnea and maintaining appropriate oxygen levels in their blood. For two years, CPAP has been used, at the MSF hospital in Khost.
“But the machines themselves are not the whole solution. What is often lacking in low resource settings are the resources. There must be enough staff to care for the patient and they must know how to use the equipment in a safe manner,” says Mats Blennow.
“Otherwise, you risk worsening the situation, or solving a problem only to create a new one. There are many home-made versions of machines that rather impair the baby's breathing ability, and if too high a concentration of oxygen, is given in the inhaled air, this can make babies blind.”
“Since there has not been enough research dedicated to the care of newborns in humanitarian crises, I can rarely use what is presented at other conferences that I participate in as a paediatrician. Many of the medical practices are still adapted to the settings in high resource countries”
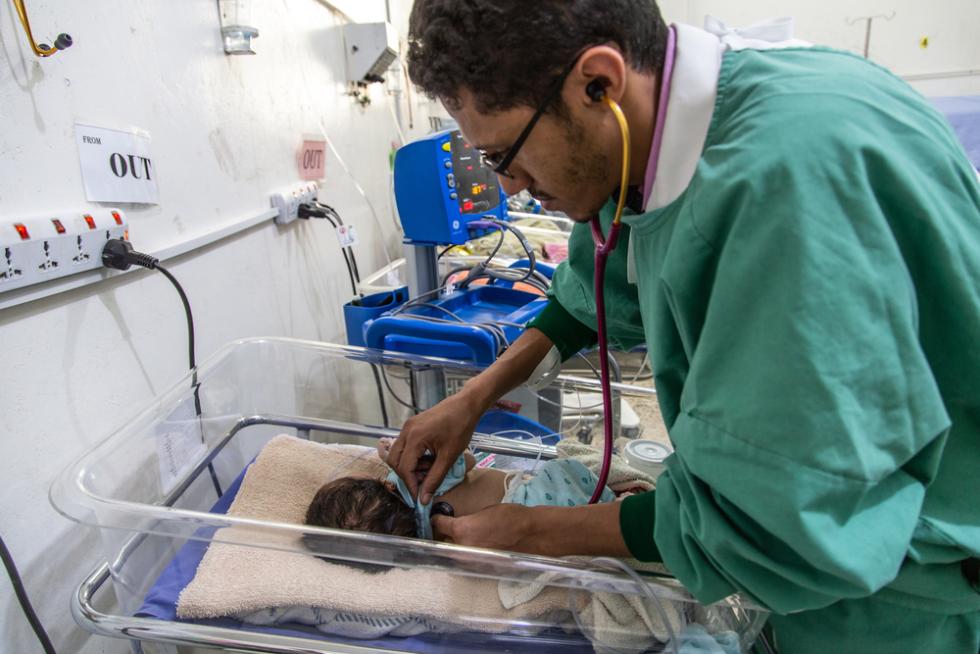
© MSF / Agnes Varraine-Leca, 2019
Mortality has gone down
Kemi Ogundipe spends a large part of her working time in hospitals and clinics around the world teaching, how to use CPAP or how to calculate the right quantity of fluid and nutrition to newborns so that they don't get too much at once – which can be very dangerous.
She is happy that the investments made by MSF in the care of newborns have yielded results. Encouraging results, indeed.
“In many of our newborn wards, the mortality rate was around 20 percent a few years ago. Last year, it had dropped to seven percent,” she says.
More research is needed
She and the others in the working group are also involved in the Paediatric Days conference organised by MSF. There, the organisation's employees and other actors gather to present new research and find new ways to collaborate around children's healthcare in humanitarian crises.
“Since there has not been enough research dedicated to the care of newborns in humanitarian crises, I can rarely use what is presented at other conferences that I participate in as a paediatrician. Many of the medical practices are still adapted to the settings in high resource countries,” says Kemi Ogundipe.
Mats Blennow and Kemi Ogundipe agree that it will take more effort to ensure that newborns everywhere in the world have a better chance of survival.
“Being a newborn is not an illness. If babies are kept warm, nourished, and protected from infections, they often become healthy people and then you have made enormous gains in the form of expected life years,” says Mats Blennow.
This article was originally published in Direkt magazine 1/2022. Text Sanna Gustafsson.
The MSF Paediatric Days are held on November 29-30 and December 1, 2022. Under the umbrella of family-centred care, the main session on 29th November will focus on newborn care. The session will introduce the concept of zero mother-baby separation and explore to what extent this concept is applied in MSF, the main barriers and challenges, and how can we overcome these by adapting the concept to fit the reality of MSF projects.
